Written by Roshini Beenukumar, PhD
Cancer cells have developed multiple mechanisms to evade the immune system. A Nature article, co-authored by a team of scientists from Basel, Tübingen, and Heidelberg, describes a mechanism by which chemotherapy-resistant leukemia stem cells evade the immune system in acute myeloid leukemia (AML) patients. These leukemia stem cells escape natural killer (NK) cells by suppressing a ligand molecule for NK cells. This study shows promise as this mechanism can be targeted by drugs that can make them immune system-susceptible. These results may also be the foundation for a new treatment approach against AML.
How do cancer cells evade the immune system?
Cancer cells employ multiple immune evasion strategies. Tumor cells present antigens on their surface which makes them recognizable by the immune system. This process has a downside as it generates a selection of cells that can evade this kind of immune surveillance, driven by genomic instability of tumor cells. One immune evasion strategy is the IDO (indoleamine 2,3-dioxygenase) mechanism. IDO expression is upregulated in multiple tumors and is associated with suppression of T cell immunity in cancer. Several immune cell types contribute to tumor evasion: (1) regulatory dendritic cells (DCs) and regulatory T cells (Tregs) generate tolerance to the tumor antigen, (2) myeloid-derived suppressor cells (MDSCs) produce pro-inflammatory factors that support tumor progression, and (3) mast cells are hypothesized to play a role in epithelial tumorigenesis. Thus, a combination of multiple immune evasion strategies may ultimately result in immune suppression beyond the tumor’s local microenvironment to achieve metastasis as seen in progressive cancers.
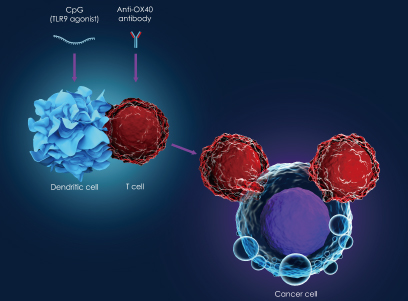
Acute myeloid leukemia and immunotherapy – current approaches
Acute myeloid leukemia, characterized by abnormal proliferation and differentiation of myeloid stem cells, is one of the first conditions where T cell-specific immunotherapy in the form of allogeneic stem cell transplant was used. Antibody-drug conjugates are also used in AML as an immunotherapy approach. This approach combines leukemia-specific antigens such as CD33 with a toxic bacterial or chemical payload, which are delivered specifically to the cancer cells. The anti-CD33 antibody-drug conjugate, gemtuzumab ozogamicin, is an approved antibody-targeted therapy for AML. Another prominent therapeutic approach is the use of T cells equipped with a chimeric antigen receptor or CAR T cells. In acute lymphoblastic leukemia (ALL) and aggressive B cell lymphomas, CAR T-cell therapy shows a high response rate. Some early studies are underway to evaluate the use of CAR T-cell therapy for AML.
Chemotherapy-resistant stem cells – a common problem in AML
AML patients often go into remission after therapy, but they subsequently relapse. The culprit here is chemotherapy-resistant leukemic stem cells (LSCs), which evade the immune system making them resistant to therapy. Current immunotherapy approaches are inadequate in treating AML, most likely due to these LSCs that lead to relapse after treatment. This study by Paczulla and colleagues explain how this immune evasion happens.
Two key players in the cancer cell’s defense against the immune system – NKG2D-L and PARP1
NKG2D, the ‟danger detector” common to NK cells and T cells, detects and eliminates damaged, transformed, and pathogen-infected cells. It recognizes stress-induced ligands (NKG2D-L belonging to MIC and ULBP families) on these target cells. Paczulla and colleagues analyzed leukemia cells from 175 AML patients and found that these ligands (NKG2D-L) are expressed on non-stem cell AML cells but not on leukemic stem cells. NKG2DL-expressing AML cells are eliminated by NK cells, whereas the NKG2DL-negative leukemic stem cells evade this killing mechanism. These leukemic stem cells are characterized by their immature morphology, molecular and functional stemness, and ability to survive chemotherapy in patient-derived xenotransplant models. "An essential mechanism of this immune resistance in leukemia stem cells is apparently the suppression of danger signals such as NKG2D-L on the cell surface", says one of the three corresponding authors of the study, Dr. Helmut Salih from the University Hospital of Tübingen and the German Cancer Consortium DKTK. Another highlight of the study is that the researchers were able to decipher the connection between stemness and immune evasion. "Such a connection between stem cell properties and the ability to escape the immune system was unknown until now," says another co-corresponding author of the study, Dr. Claudia Lengerke from the University Hospital of Basel and the University of Basel.
What is the mechanism behind this immune evasion strategy?
This is where the second key player in this defense mechanism comes in – PARP1. Poly-ADP-ribose polymerase 1 (PARP1), which plays a prime role in DNA damage repair and maintenance of genome integrity, is implicated in multiple cancers. Several PARP inhibitors are approved for clinical use such as Olaparib (KuDOS/AstraZeneca) for the treatment of advanced-stage BRCA1/2-mutated ovarian cancer. The immune evasion strategy employed by NKG2DL-negative leukemic stem cells seems to be mediated by PARP1.
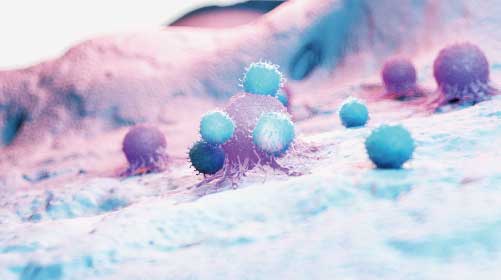
PARP1 expression is upregulated in leukemic stem cells which represses NKG2D-L expression leading to immune evasion. In patient-derived xenotransplant mice models treated with PARP1 inhibitors, leukemic stem cells regained their ability to express NKG2D-L. The subsequent transfer of polyclonal NK cells in these models suppressed tumor formation as these stem cells were recognized and eliminated by NK cells.
Future directions
The involvement of PARP1 in this immune evasion mechanism is particularly interesting. PARP1 inhibitors are well tolerated in these mouse models of AML and more importantly in cancer patients. PARP1 inhibitors in combination with other treatments may allow specific leukemic stem cell-targeting, which would one day help us achieve a long-term cure for AML.
"Our results show how cancer stem cells cleverly trick the immune system. The elucidation of the underlying mechanism now makes it possible to counterattack," says the third co-corresponding author of the study, Dr. Andreas Trumpp, German Cancer Research Center and HI-STEM
In conclusion, this study elucidates a novel mechanism by which leukemia stem cells evade the immune system. The involvement of PARP1 in this mechanism opens a new door – the possibility to combat these chemotherapy-resistant stem cells by combining PARP inhibitors with active NK cells. The scientists involved in the study are gearing up for a clinical study to evaluate and validate these findings in a clinical setting.
"Stay informed with the latest news from PHCbi”
Reference
1. Making cancer stem cells visible to the immune system: New results may enable innovative treatment concept against leukemia. ScienceDaily https://www.sciencedaily.com/releases/2019/07/190717132812.htm.
2. Paczulla, A. M. et al. Absence of NKG2D ligands defines leukaemia stem cells and mediates their immune evasion. Nature 572, 254–259 (2019).
3. De Kouchkovsky, I. & Abdul-Hay, M. ‘Acute myeloid leukemia: a comprehensive review and 2016 update’’’. Blood Cancer J. 6, e441 (2016).
4. IDO inhibitors in advanced melanoma: A path forward? oncology.medicinematters.com https://oncology.medicinematters.com/melanoma/ido-inhibitors/ido-inhibitors-in-melanoma--a-path-forward-/16410630 (2019).
5. Prendergast, G. C. Immune escape as a fundamental trait of cancer: focus on IDO. Oncogene 27, 3889–3900 (2008).
6. Naval Daver, M. D. Immunotherapy Approaches in AML. Cancer Network https://www.cancernetwork.com/article/immunotherapy-approaches-aml (2019).
7. Liu, Y., Bewersdorf, J. P., Stahl, M. & Zeidan, A. M. Immunotherapy in acute myeloid leukemia and myelodysplastic syndromes: The dawn of a new era? Blood Rev. 34, 67–83 (2019).
8. Griffin, G. K. Leukemic stem cells hiding in plain sight. Sci. Immunol. 4, eaay7253 (2019).
9. Zingoni, A. et al. NKG2D and Its Ligands: “One for All, All for One”. Front. Immunol. 9, (2018).
10. Zeniou, M., Nguekeu-Zebaze, L. & Dantzer, F. Therapeutic considerations of PARP in stem cell biology: Relevance in cancer and beyond. Biochem. Pharmacol. 167, 107–115 (2019).